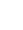Council of Councils global perspectives roundups gather opinions from experts on major international developments. In this edition, members from leading global think tanks in Italy, China, Singapore, India, and the United Kingdom reflect on the coronavirus (COVID-19) pandemic, the state of public health systems in their countries, and the importance of international and regional cooperation.
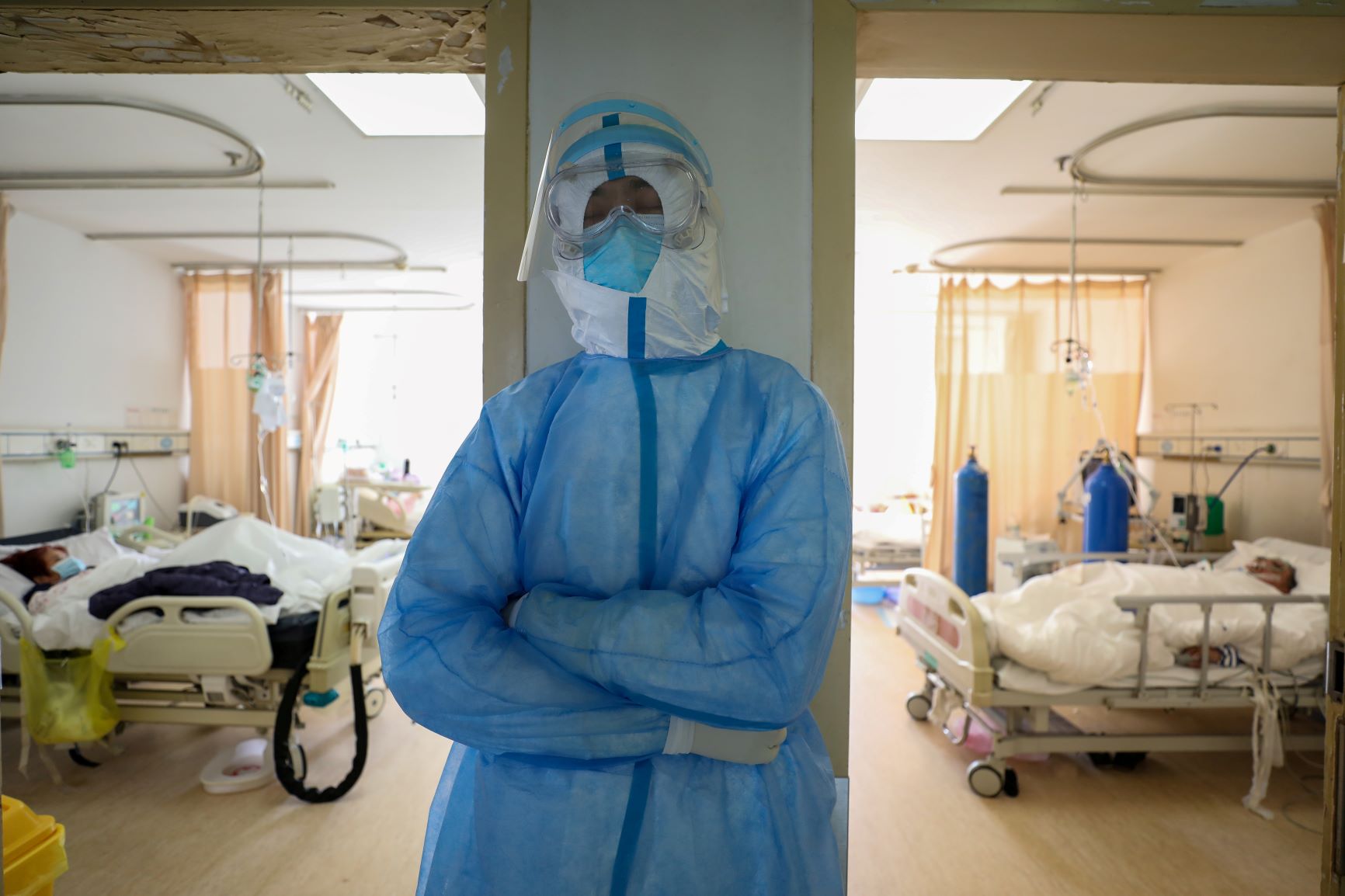
Italy’s Hard Lessons
Italy’s health-care system is almost unique in that it guarantees care to all citizens. In outbreaks of highly contagious diseases such as the new coronavirus, COVID-19, universal coverage contributes to better monitoring and containment of infections. It is also—critically—socially fair. That said, the Italian health-care system has fundamental weaknesses. Following the outbreaks of other epidemics—SARS, MERS, avian flu, Ebola, and Zika—Italy took steps to devise contingency plans but never went further than broad guidelines, and certainly never developed plans for an emergency like COVID-19.
A further problem has been the insufficient level of communication and coordination between the central government in Rome and regional authorities, which have a constitutional responsibility to organize health-care structures and provide care services. This has sometimes resulted in confusing public messaging, whereas clarity is of the utmost importance in discouraging social habits and personal behavior that might facilitate the spread of the disease.
The Italian government’s decision to enact severe restrictions on all nonessential economic activity, as well as the movement of people across the whole country, responds to the dual purpose of containing the spread of the contagion while preserving hospitals’ capacity to provide care for the infected, whose numbers have been growing at an alarming pace over two weeks. Today, only pharmacies, food stores, and a few other shops remain open, and Italians are allowed to leave their homes only for reasons of proven necessity, such as work, provision of food and medicine, and demonstrable emergencies. Italy is thus emerging as a testing ground for other countries in Europe that are also recording growing numbers of infected people. Hopefully, this could prompt the European Union to step up cooperation and mutual support, for instance, by facilitating transfers of critical medical equipment such as masks and respirators to Italy.
The combination of high population density, social inequality, and mobility will provide a fertile ground for epidemics to spread and jeopardize global health and economic growth. To better face them, we should learn the lessons from the COVID-19 experience: contingency plans, easy access to health care, coordination among health authorities, clear public messaging, corporate and individual responsibility, and mutual support among nations (especially in the EU).
Bridging Shortfalls in International Cooperation
Is the fast-spreading COVID-19 pandemic a wake-up call for countries to act swiftly and in concert to build a safer, globalized world? The answer is contingent upon whether all countries reach a consensus and establish joint mechanisms to deal with major public health emergencies.
The unfolding crisis has exposed many flaws and vulnerabilities in the world’s public health emergency preparedness. Countries differ starkly in their political and value systems, social norms, culture and traditions, regional and global security risks, exposure to global health risks, and health emergency preparedness and capacity. Given these differences, a health emergency in one country may trigger different reactions and responses across the world, making consensus-building difficult and international coordination even more difficult.
To address these challenges, we must first update our outmoded concept of health security to overcome a lamentable “cycle of panic and neglect.” Second, we must mend the flawed health-emergency response mechanisms and build up monitoring and response capabilities in developing countries so that International Health Regulations can be followed amid health crises. Third, we must strengthen global leadership and bridge resource shortfalls in international health cooperation, and make earnest efforts to counter politicization and stigmatization of health crises. Fourth, we must increase the sharing of best practices on public health emergency responses so that the world does not have to start from scratch in every crisis.
As the main battlefront of the global antivirus war, China has made the greatest efforts, taken the strictest measures, gained the most firsthand experience, and achieved the most remarkable results by far. Many Chinese practices have been commended by the World Health Organization (WHO), including its whole-of-society mobilization system, unprecedented social-distancing measures, timely information and knowledge sharing with the WHO, and deep involvement in international medical research cooperation.
The WHO has just declared COVID-19 a pandemic. Viruses respect no borders. Humanity’s past encounters with viruses and epidemics have proven and will prove again that empathy, solidarity, and coordination are the only rational response to massive outbreaks of infectious diseases and will lead us to a safer, globalized world with a shared future.
The Pandemic Preparedness Fatigue Problem
Pandemic outbreaks are grim reminders of how public health issues are critical to global security. The world is grappling to contain the spread of COVID-19 and deal with its severe effects on economies, its disruption of people’s lives, and the acute psychosocial stresses it places on society. The numbers tell the story. While COVID-19 cases in China, the epicenter of the disease, have started to peak from a high of more than eighty thousand cases, we see the opposite trend in other regions. Parts of Europe (particularly Northern Italy), North America, and Southeast Asia report rising cases as governments come under pressure to conduct extensive testing. In Southeast Asia, experts have warned that the outbreak will not end soon and that the health crisis may be prolonged.
Agreement for greater multilateral cooperation is urgently needed to collectively respond to the COVID-19 outbreak. The crisis also provides yet another opportunity to reexamine the serious structural issues that hinder effective international efforts to prevent, detect, and respond to infectious diseases.
Pandemic outbreaks are not a twenty-first century problem. There are historical precedents that have well-established their threat to global security, such as plagues, Spanish flu, SARS, and H1N1. In today’s globalized environment, growing connectivity and the wonders of technological advances should have already accelerated and strengthened international efforts for pandemic preparedness. That pandemic preparedness fatigue was observed to have set in after the SARS and H1N1 crises is indeed instructive. This could perhaps explain why much of the world was caught unprepared to robustly contain the emergence of a new pathogen.
The world should not miss this chance to jointly address the challenges to global health security. The agenda for action includes: calibrating the implementation of International Health Regulations; narrowing disparities in health-care systems; strengthening national and local public health systems’ capacities for disease surveillance and reporting, laboratories, and diagnostics; beefing up hospitals’ surge capacities in times of emergencies; and providing access to vaccines and other medicines.
Timely national and regional actions are also extremely critical. By early March, Singapore’s decisive whole-of-government approach to containment and mitigation, with effective risk communication strategies, has significantly changed the nation’s climate of uncertainty and fear to public confidence in the government. Singapore and its counterparts in the Association of Southeast Asian Nations (ASEAN) have also been strengthening regional efforts to fight the disease. Multilevel and multisectoral coordination, as well as sustained regional and international commitments, are crucial pillars to ensure global health security.
An Old Scourge in a New, Uncertain Age
Having dawdled for weeks, the WHO has finally declared the COVID-19 outbreak a global pandemic. Given that it is too soon to assess how well global institutions and governments have responded to the emerging public health challenge, that discussion is best left for another day. For the moment, three facets of COVID-19 merit comment.
First, we are witnessing what can be described as an “infodemic.” Thanks to social media platforms and an attention-hungry mainstream media, there is an overflow of (mis)information about COVID-19. For many, it can be hard to determine what is true and what is false since exaggeration is the new normal. The relatively restrained public discourse over HIV when it first made its appearance stands out in sharp contrast.
Second, the COVID-19 outbreak proves again that history tends to repeat itself. This is not the first time a killer virus has traveled along connected networks. Nor is it the first time that travelers have carried a virus. Colonial settlers carried gonorrhea, smallpox, and other diseases to the New World. Ships carried plague-infested rodents to foreign shores. Given China’s central role in the global economy and the outward flow of its tourists and labor through the Belt and Road Initiative, what would have once been a local epidemic, like the 2003 SARS outbreak, is now a global health crisis.
Third, COVID-19 has added a twist to emerging political realities. Will China reconsider its ruler-for-life decision or has Chinese President Xi Jinping demonstrated the benefit of opting for a reliable authoritarian system? Will American elections be altered by the national outbreak response and its seemingly significant economic implications? Will the EU be forced to rethink its immigration policy? As China provides aid to Italy and other affected countries, will we see a red dawn of another hue? These uncertainties will mutate for a long time even after the macabre march of the virus has been contained, if not halted.
The UK’s Public Health Agencies Are Ready
The United Kingdom has been preparing for years to be able to respond as effectively as possible to an outbreak such as COVID-19. Its public health agencies are central to the current response, and they are working closely with the National Health Service (NHS) and others to ensure all necessary actions are taken. There is a high level of trust in the NHS’s publicly financed services, which ensure rapid access to preventive and curative care. UK public health agencies are also highly regarded worldwide and have an excellent track record of managing infectious disease emergencies.
The response to COVID-19 in the UK benefits from extensive cross-government and cross-sectoral planning and preparation, with plans strengthened by testing and exercising at all organizational levels.
The UK has strong expertise and experience in the areas essential to informing preparedness and response. For example, as a world leader in outbreak modeling, it can use state-of-the-art models to assist decision-making in real time. Modeling has also helped inform preparations for a “reasonable worst case” scenario, designed to improve the UK’s ability to respond to different situations should the virus spread widely throughout communities.
The framework for international cooperation has been built and refined over a long period of time, evolving from lessons learned during previous emergencies such as the 2009 H1N1 flu pandemic and the 2014–2016 Ebola outbreaks. Many assessments informed this learning, including those by specially constituted International Health Regulations Review Committees, which reported their findings directly to the WHO’s World Health Assembly. This framework is critical to the rapid sharing of information between countries and agencies and in the development of diagnostics, therapeutics, and vaccines. In this context, the WHO is providing leadership by working closely with member countries, particularly in technical and scientific areas.