Major Pandemics of the Modern Era
1899 – 2025
For more than a century, countries have wrestled with how to improve international cooperation in the face of major outbreaks of infectious diseases. The COVID-19 pandemic, which brought the world to a near halt in 2020 and killed nearly seven million people, underscored the urgency.

1899-1923
Sixth Cholera Pandemic

A new outbreak of cholera, a bacterial infection contracted through the consumption of contaminated food and water, begins in India at the turn of the century. It’s the latest wave of a disease that has caused pandemics intermittently since the early 1800s. The outbreak spreads to Russia, as well as to parts of the Middle East and North Africa, ultimately killing hundreds of thousands of people—with particularly high death tolls in India and Russia. Advancements in sanitation and public hygiene are credited with preventing the pandemic from taking hold in Europe and North America.
1918–1920
Spanish Flu Engulfs the Globe
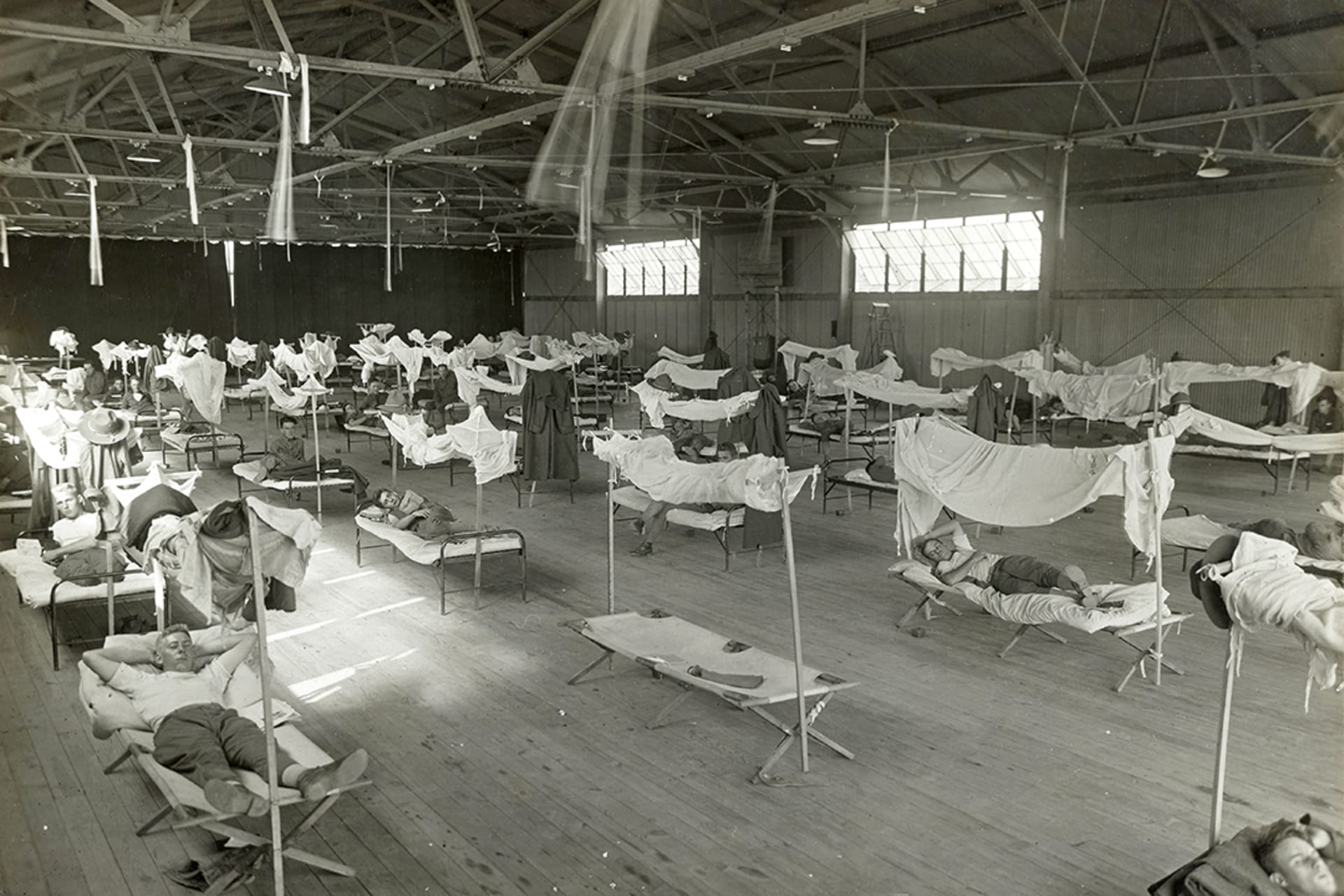
A new influenza virus begins to spread worldwide amid the upheavals of World War I. There is no consensus on the origin of the pandemic, but it is first publicly reported in Spain. It infects an estimated five hundred million people, roughly one-third of the world’s population at the time, and kills some fifty million, with an unusually high fatality rate among otherwise healthy young adults. Many governments look to isolation measures, quarantines, and disinfecting efforts, but the global movement of troops hinders containment. At the time, there is no flu vaccine and antibiotics have not yet been developed to treat secondary bacterial infections. In the United States alone, about 675,000 people die, lowering the country’s average life expectancy by more than twelve years.
1928
Penicillin Ushers in Antibiotics Era

Scottish scientist Alexander Fleming discovers penicillin, the first antibiotic—a class of drugs used to treat bacterial infections—marking a major milestone for global health. Widespread use of antibiotics takes off in the early 1940s during World War II. They soon become the go-to treatment for common illnesses, such as strep throat and urinary tract infections, and significantly reduce the death rates for many ailments, including syphilis and tuberculosis.
1948
Creation of the WHO

The constitution of the World Health Organization (WHO), signed by more than sixty countries, enters into force in April 1948. The body, a part of the newly formed United Nations, sets out to coordinate international health policy, seeking to combat diseases such as malaria and tuberculosis and improve sanitation practices. The WHO builds on previous agencies including the League of Nations’ Health Organization (1920–1948), as well as earlier initiatives such as the International Sanitary Conferences, the Pan American Health Organization, and the International Office of Public Hygiene, which beginning in the nineteenth century issued regulations to improve health standards and prevent the spread of diseases such as cholera and yellow fever.
1957–1958
Asian Flu Pandemic

A new strain of influenza virus, designated H2N2, is reported in Singapore in February 1957, and soon spreads to China, Hong Kong, the United Kingdom (UK), and the United States. Though less severe than the Spanish Flu, the Asian Flu kills more than one million people worldwide. A second wave of cases beginning at the end of that year is particularly deadly, and young children, elderly people, and pregnant women are hardest hit. A vaccine is quickly developed in 1957, but its deployment is limited and it does little to mitigate the outbreak, experts later say.
1961–Present
World’s Longest Pandemic

A cholera pandemic originating in Indonesia spreads to other parts of Asia, the Middle East, and Africa over the course of a decade, and continues to this day. By the 1990s outbreaks also take hold in South America, the first on that continent in nearly a century. An outbreak in Zimbabwe in 2008–09 kills more than four thousand people, and major outbreaks in Haiti and Yemen each affect more than a half million people. Some three million people are infected with the bacteria that cause cholera each year, and it remains endemic in close to fifty countries. Health experts say oral cholera vaccines, introduced in the 1990s, are not a replacement for improved sanitation.
1968–1969
Hong Kong Flu Pandemic

A decade after the Asian Flu, a new strain called H3N2 emerges. Commonly called the Hong Kong Flu, it emerges first in Hong Kong, then a British colony, in July 1968. It soon travels across East and South Asia, then to Australia, Europe, and North America, and on to Africa and South America by 1969. U.S. troops returning from the Vietnam War are believed to have brought the virus to the United States. An estimated one million people die in the pandemic, about half of them Hong Kongers and many of them people sixty-five years of age or older. Descendants of the H3N2 virus continue to circulate seasonally worldwide.
1977–1980
Smallpox Eradicated

The last known case of smallpox, a viral disease that plagued humans for millennia, is diagnosed in 1977 in Somalia, following a nearly two-decade-long global vaccination campaign. Three years later the WHO formally declares it eradicated around the globe. The elimination of the disease, which was fatal in as many as one-third of patients, marks unusual U.S.-Soviet cooperation during the Cold War. It also highlights major advancements in the study and use of vaccines: polio vaccines introduced in the 1950s and 1960s lead to similar success globally, and vaccines are credited with reducing rates of illnesses such as measles, diphtheria, and whooping cough to all-time lows.
1981–Present
HIV/AIDS Pandemic
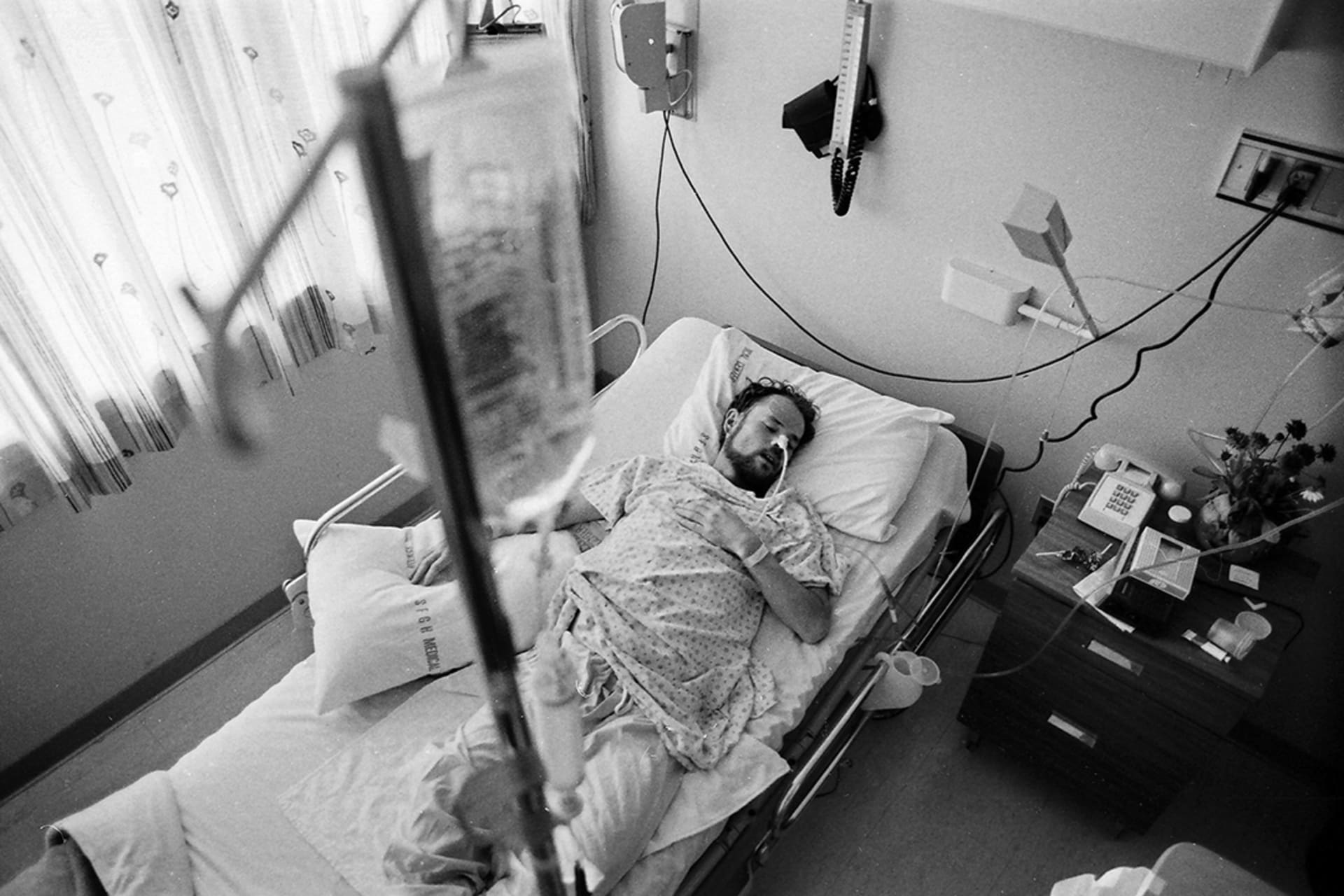
A 1981 report by what is now the U.S. Centers for Disease Control and Prevention (CDC) describes a rare form of pneumonia that is later identified as Acquired Immunodeficiency Syndrome, or AIDS. It is the most advanced stage of Human Immunodeficiency Virus (HIV). This marks the start of an explosive growth of cases, and by the early 1990s AIDS becomes the leading cause of death in men between the ages of twenty-five and forty-four in the United States. In 1996, the United Nations establishes UNAIDS to coordinate global action. The introduction of antiretroviral therapy helps to bring down the U.S. death toll, but the epidemic grows across Africa. The 2003 U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) boosts international funding, and between 2000 and 2018 HIV-related deaths decrease by 45 percent. Today, close to forty million people have HIV/AIDS, more than two-thirds of whom are in sub-Saharan Africa. Tens of millions of people have died from the disease.
2002–2003
SARS Emerges in China

The Severe Acute Respiratory Syndrome (SARS) coronavirus, part of a family of viruses that commonly cause respiratory symptoms such as coughing and shortness of breath, is first identified in late 2002 in southern China. SARS spreads to more than two dozen countries across four continents, infecting more than eight thousand people. In March 2003, the WHO triggers its Global Outbreak Alert and Response Network (GOARN) to coordinate research by teams of international experts and the deployment of supplies and health workers to affected countries. Health experts sharply criticize Beijing for covering up the initial spread of the virus. SARS kills close to eight hundred, most within China and Hong Kong, by the time the outbreak is quelled in mid-2003. The virus is thought to have been transmitted to humans via contact with civet cats.
2005
WHO Writes New Rules

The WHO rewrites its International Health Regulations, rules originally drawn up in 1969 that are binding on all WHO member states. The new rules aim to boost collective defenses against global health challenges and improve pandemic preparedness and response. Entering into force in June 2007, they require states to notify the WHO of potential global health emergencies. They also grant the WHO director-general the authority to declare a public health emergency of international concern, or PHEIC, in order to mobilize a global response. The changes are meant to build on the GOARN established in 2000.
2009–2010
U.S. at Center of H1N1 Pandemic
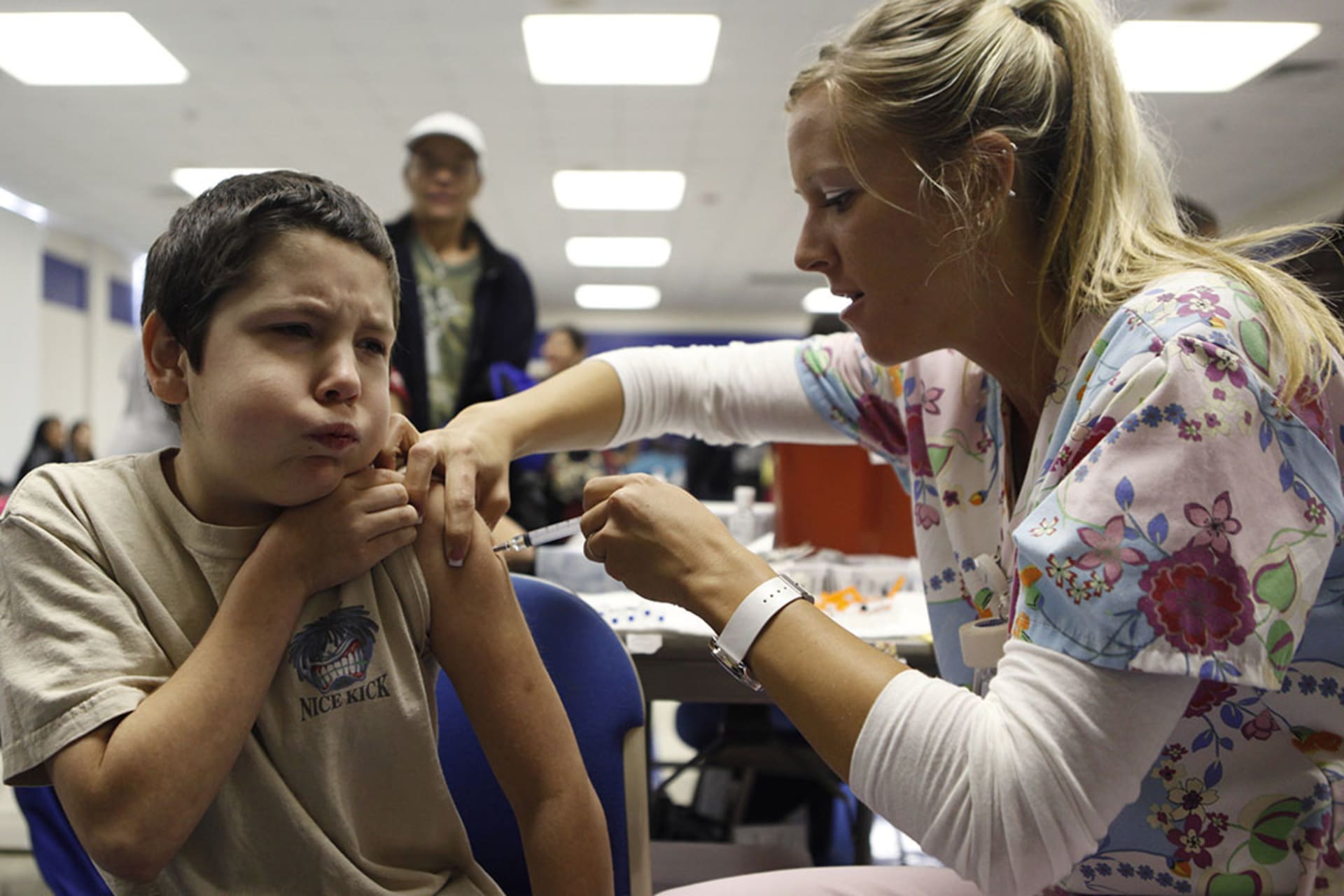
A new influenza virus, labeled H1N1 and commonly referred to as the swine flu because of its links to influenza viruses that circulate in pigs, begins to spread in early 2009 in Mexico and the United States. Unlike other strains of influenza, H1N1 disproportionately affects children and younger people. The CDC calls it the “first global flu pandemic in forty years.” The WHO declares a PHEIC in April 2009, then designates the spread of H1N1 a pandemic in June, after the virus reaches more than seventy countries. In response, some countries advise against travel to North America, and China imposes mandatory quarantines for patients and their close contacts. The CDC estimates that between 151,700 and 575,400 people die worldwide—around 12,500 in the United States—in the first year after the virus is discovered. Around 80 percent of those who die are younger than sixty-five. The WHO announces the pandemic’s end in August 2010, though the strain continues to circulate seasonally.
2012
MERS Uncovered in Middle East

A new coronavirus, named Middle East Respiratory Syndrome (MERS), is transmitted to humans from camels in 2012 in Saudi Arabia. The largest outbreak occurs on the Arabian Peninsula in the first half of 2014, with the Saudi city of Jeddah as its epicenter. In 2015, South Korea is home to the second-largest outbreak. More than two dozen countries report cases of the viral respiratory disease in the following years, though the majority of cases are in Saudi Arabia. The virus commonly causes pneumonia in those infected and has a relatively high fatality rate: of the roughly 2,500 people diagnosed with MERS since its discovery, more than 850 have died from the disease.
2014
Uptick in Polio Prompts WHO Emergency

In May 2014, WHO Director-General Margaret Chan declares a PHEIC over a rise in polio cases in Africa and Asia. The virus, which paralyzed or killed hundreds of thousands of people yearly at its peak, had been nearly eradicated after mass vaccination campaigns starting in the late 1950s. The disease, which disproportionately affects young people, proves hard to eliminate completely, particularly in conflict zones. Widespread mistrust of vaccination programs is a major challenge. As of 2022, the PHEIC over the possible spread of polio remains in place, and the disease is still endemic in Afghanistan and Pakistan.
2014–2016
Ebola Sweeps West Africa

In early 2014, cases of the Ebola virus, a rare and severe infectious disease that leads to death in roughly half of those who contract it, are detected in Guinea and soon after in Liberia and Sierra Leone. It is the first time the disease moves into densely populated urban areas, allowing for rapid transmission. The outbreak eventually spreads to seven other countries, including several European states and the United States, causing more than eleven thousand deaths in all. Mistrust of health workers and rumors again present challenges to containment. The WHO, which declares the outbreak a PHEIC in August 2014, is criticized for what many call a slow response. In September 2014, the UN Security Council adopts a resolution calling on member states to pool global resources to combat the crisis, and countries including the United States and the UK deploy health workers and other aid. The hardest-hit countries declare themselves Ebola-free in June 2016.
2015
Fight Against Mosquito-Borne Diseases Continues

The WHO reports in 2015 that malaria infections are down by more than one-third globally compared to 2000, as the United Nations and the Bill & Melinda Gates Foundation launch a major joint effort to eradicate the disease by 2040. Malaria still kills several hundred thousand people yearly, two-thirds of whom are children under five. Eradication efforts focus on the eleven countries where the large majority of malaria cases occur, all of which are in sub-Saharan Africa except for India. Meanwhile, cases of dengue, another mosquito-borne disease, spike between 2000 and 2015, partly due to increased reporting. Dengue is endemic in more than a hundred countries, with the majority of the 100–400 million yearly cases occurring in Asia. These diseases have proven difficult to eliminate, as researchers confront numerous challenges to developing successful vaccines.
2015–2016
Zika Spreads Across Americas

An outbreak of the Zika virus, first discovered in Uganda in the 1940s and transmitted mainly by mosquitoes, takes off in Brazil in early 2015. In February 2016, the WHO declares the outbreak a PHEIC, and by the middle of the year more than sixty countries report cases of the virus, including the United States. Thousands of women infected with the virus while pregnant give birth to babies with microcephaly, a condition in which a child’s head is smaller than normal, and other congenital conditions. Some governments urge women to delay pregnancy amid the outbreak. Despite calls for cancellation, the 2016 Summer Olympics in Rio de Janeiro go ahead as planned. The WHO declares the end of the epidemic in November 2016.
2018–2020
Ebola Returns in Conflict-Stricken Congo

In August 2018, the Democratic Republic of Congo (DRC) declares an outbreak of the Ebola virus in the country’s northeast. Several cases are later reported across the border in Uganda. Protracted conflict in the area hampers the response, as health workers face attacks by armed groups; misinformation and mistrust among the local population are also challenges. By June 2019, the Ebola outbreak becomes the second largest in history, and in July the WHO declares a PHEIC, urging increased international support to end the crisis. More than 3,400 people are infected with the virus, and close to 2,300 die. In June 2020, nearly two years after the outbreak’s start, the WHO declares it over. However, smaller outbreaks continue to crop up in parts of the country.
2019–2023
COVID-19 Runs Rampant
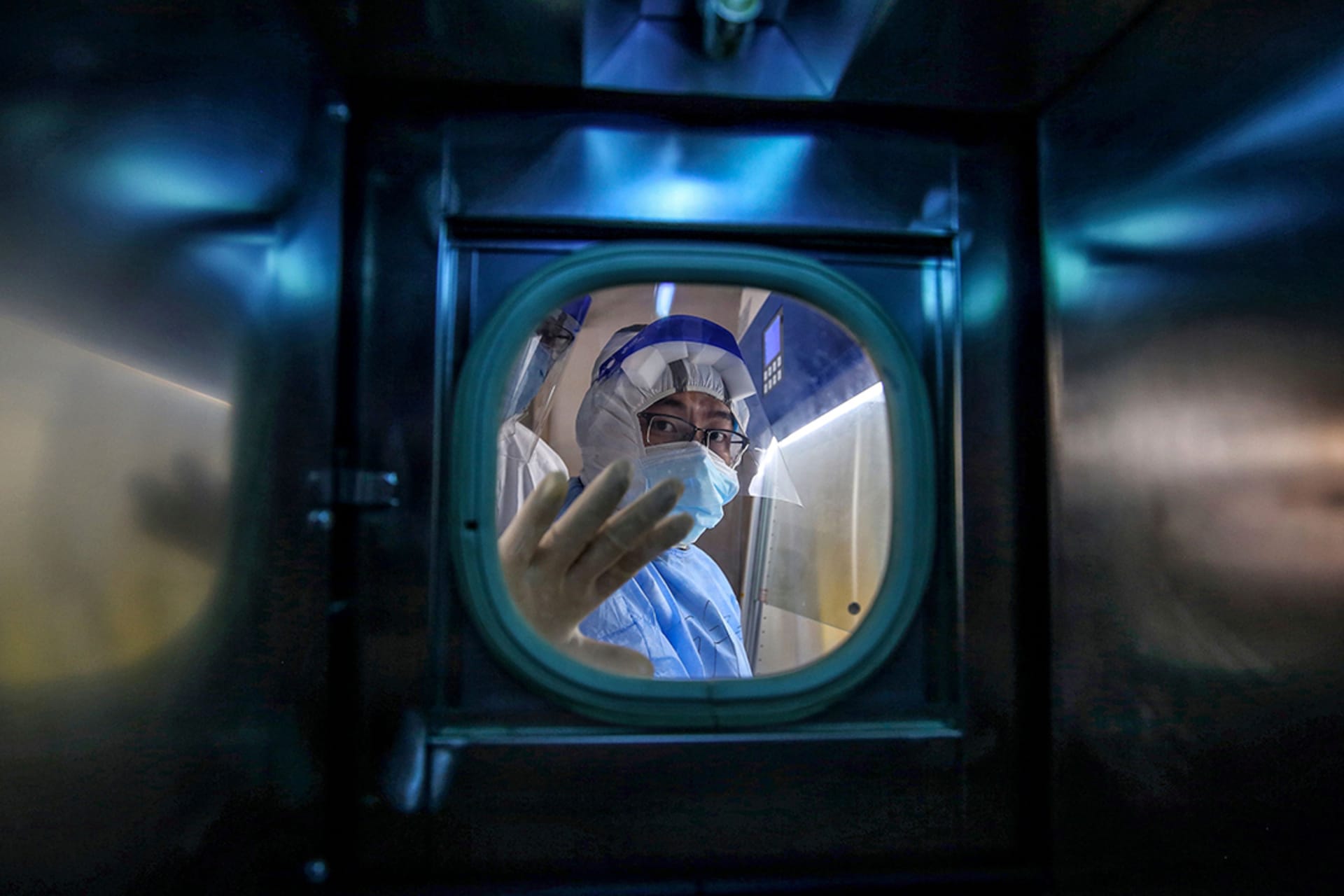
A new coronavirus emerges in China’s Hubei Province in late 2019, spreading rapidly to other parts of China. The virus soon travels throughout the rest of the world, and in January 2020, the WHO designates the outbreak a PHEIC. Many governments impose restrictions to try to stop its spread, including lockdowns, mandates to wear face masks, limits on large gatherings, and quarantines for people who are infected. After three years, the official WHO death toll from the COVID-19 disease nears seven million people, though the actual number is believed to be up to three times higher. The economic decline is described as the worst since the Great Depression, with supply-chain and labor-force disruptions reverberating worldwide. At the same time, the world marks the fastest-ever development of safe and effective vaccines. However, uneven vaccine distribution and the emergence of more dangerous variants frustrate global efforts to end the pandemic. In May 2023, with 70 percent of the global population having at least one vaccine dose and a decline in COVID-19-related deaths and hospitalizations, the WHO director-general lifts the PHEIC, calling for a transition to long-term management of the pandemic.
2022–2023
A Race to Contain Mpox

A case of mpox, formerly known as monkeypox, a rare zoonotic virus, is reported in the UK in May 2022. The virus is similar to smallpox, because it leads to some of the same symptoms and both are from the orthopoxvirus family. However, mpox is considered less transmissible and less fatal. The virus spreads rapidly in countries where it is not endemic; by July, there are around sixteen thousand reported cases and three confirmed deaths, and the disease is present in at least seventy-five countries. In an unusual move, WHO Director General Tedros Adhanom Ghebreyesus declares it a PHEIC despite a lack of consensus among a WHO emergency committee. Though cases are primarily among men who have sex with men, the WHO chief warns that the risk of infection extends to other communities. Because smallpox vaccines can be used to fight mpox, countries work to expand their limited availability. A rapid global response to the outbreak leads its spread to slow significantly by May 2023, with 87,000 reported cases and 140 confirmed deaths across 111 countries. That month, the WHO declares that mpox is no longer a public health emergency.
2025
March 2025
Five Years Post-COVID, Global Divide Still Seen on Pandemics

Five years after the start of the COVID-19 pandemic that killed an estimated seven million people worldwide, global health leaders remain divided on a future pandemic response. While the WHO has been leading talks on a Pandemic Agreement since 2021, countries cannot reach a consensus on many of its provisions, including vaccine and technology equity, information sharing, and primary prevention tactics. Meanwhile, the United States, once the lead financial contributor to global public health efforts, pulls away from cooperation after President Donald Trump again withdraws from the WHO. His administration also halts large swaths of foreign aid, which experts say is critical to fighting disease outbreaks around the world. Trump appoints Robert F. Kennedy Jr.—a known vaccine skeptic—as the top ranking health official in his cabinet.