Health
Archive
1124 results
- Workshop
2026 Local Journalists Workshop
 By Surina Venkat
By Surina Venkat- Task Force Report
U.S. Economic Security

- Backgrounder
Fentanyl and the U.S. Opioid Epidemic

- Backgrounder
What Does the CDC Do?

 By Thomas J. Bollyky
By Thomas J. Bollyky- Backgrounder
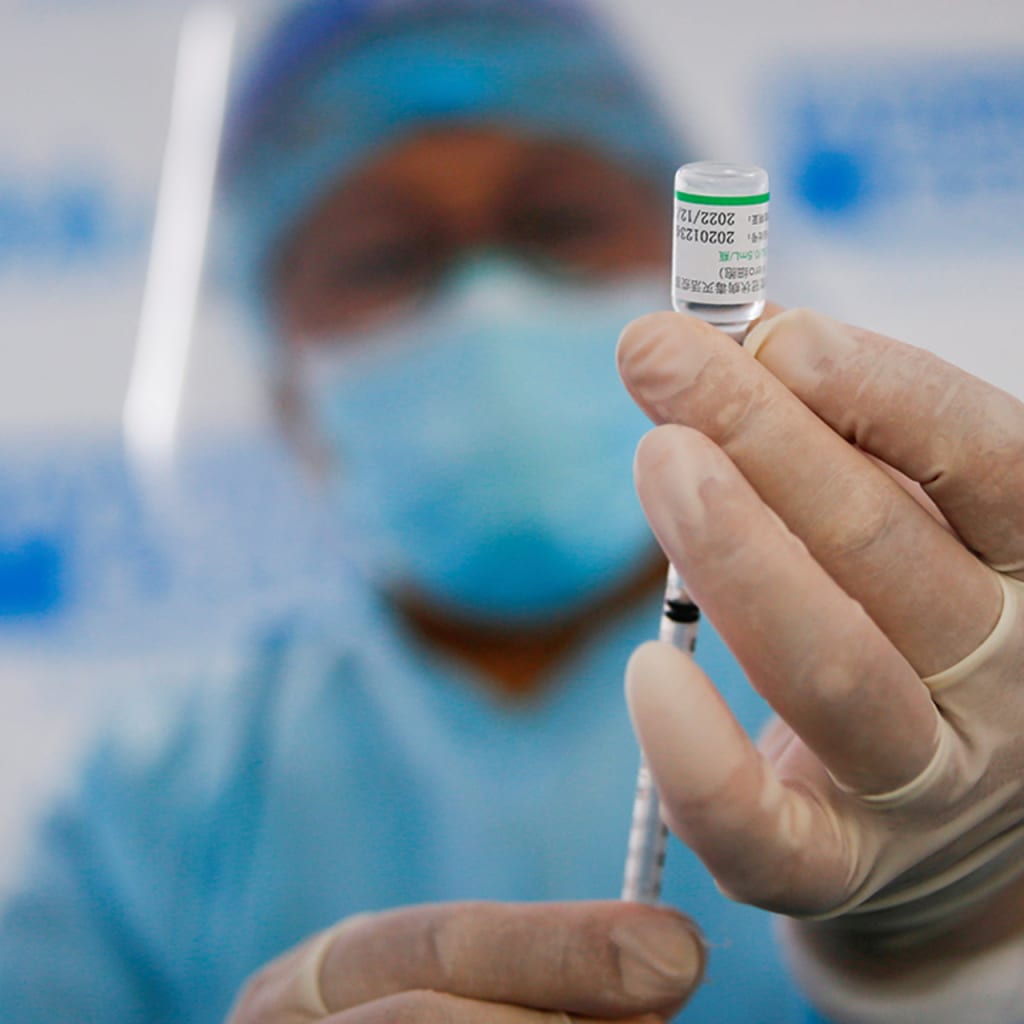
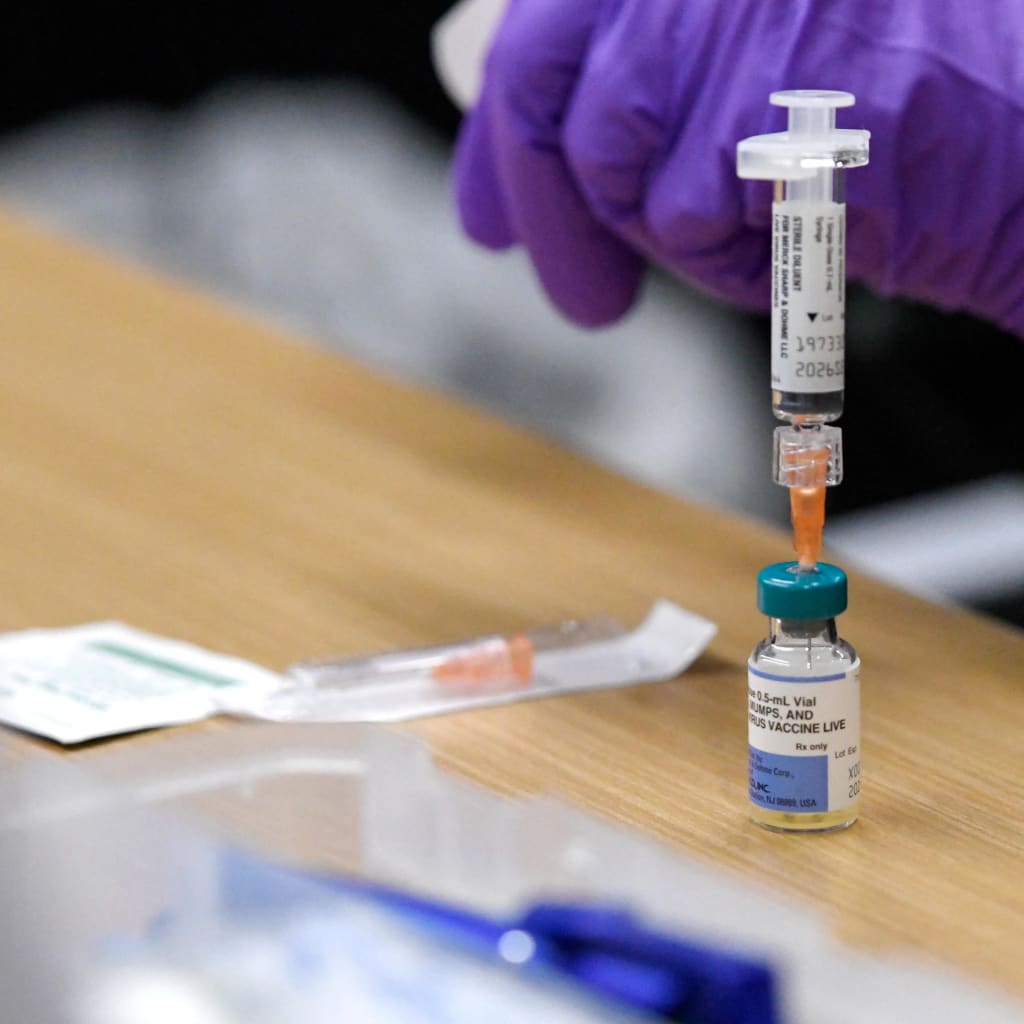
How Vaccines Changed the World

 By Ellora Onion-De
By Ellora Onion-De By Linda Robinson and Noël James
By Linda Robinson and Noël James